Communication in the ED: A Key Satisfaction Metric
In hospitals everywhere, one medical specialty has been particularly impacted by the long tail of the COVID-19 pandemic: the Emergency Department (ED).
Although ambulances are no longer lining up to deliver streams of severely ill patients with COVID-19 to the ED, medical professionals who work inside the ED — and patients who visit the ED for care — continue to feel the brunt.
Yet ongoing studies point to one factor that has a tangible impact on ED patient satisfaction, and it’s not a piece of high-tech equipment or a new medical technology.
It’s communication.
Several recent medical studies highlight the value of patient-provider communication in the ED. Using very different approaches, the researchers found that keeping patients informed can be an interpersonal antidote to common ED challenges and frustrations, including long wait times, overcrowding, and satisfaction scores.
Provider-Patient Communication: A Measurable Commodity
The first study, 1 done in 2022 in cooperation with the Centers for Medicare and Medicaid Services (CMS), identified four factors that should be included in CMS-mandated surveys of discharged ED patients; three of the factors involved some sort of communication.
In addition to getting timely care, the researchers identified “how well doctors and nurses communicate,” “communication about medications,” and “communication about follow-up” as meaningful measures for monitoring the quality of care provided and for boosting patient satisfaction scores.
A second study2 by Canadian medical and art/design experts identified environmental factors that impact patients’ experiences in the ED. One of the most commonly identified factors in the 2022 study? Communication, which ranked with overcrowding, wait times, and privacy.
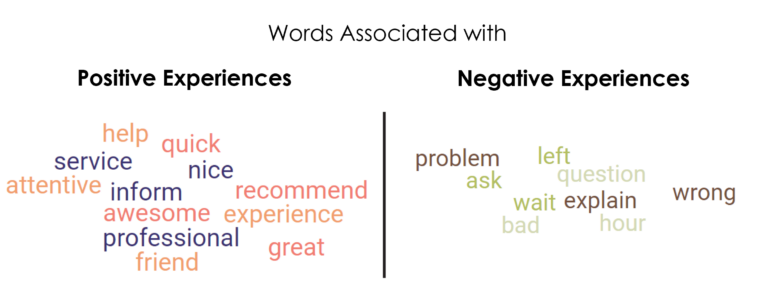
And a third multi-center study,3 also from 2022, “The Emergency Department Patient Experience: In Their Own Words,” used visualization software to create word clouds, based on frequently occurring words and phrases in ED patients’ survey responses after they were released from the ED.
- Words associated with positive experiences included: inform, professional, service, nice, attentive, friend, help, experience, recommend, great, awesome, quick
- Words associated with negative experiences included: wait, ask, left, hour, never, bad, question, wrong, problem, explain, question
During a patient’s ED stay, the researchers recommend frequent updates about when patients will be seen, frequent re-evaluations during their ED stay, and sharing of test results to help patients take ownership of their care and improve survey scores.
A New ED Role: Patient Experience Coordinator
ApolloMD’s recent implementation of a patient experience coordinator in a partner hospital’s ED is one solution to patients’ expectations for ongoing, informative communication.
Indeed, patient satisfaction scores rose at one partner hospital that embraced the value of improved communication in the ED. The Florida hospital placed an ApolloMD-trained Patient Experience Coordinator (PXC)—a new role—in its busy emergency department. The PXC served as a personal liaison between the medical team and patients, both in the waiting room and in treatment rooms.
After just six months of the PXC’s presence in the ED, 99% of patients described the ED team members as professional and courteous, 93% knew who their caregiver was, and 92% felt the ED team was addressing their concerns. Likewise, the department’s percentile ranking of likelihood of patients recommending care to others rose from 21 to 71.

In that hospital, communication played a huge role in improving the ED experience and scores.
Does your ED need new solutions to manage staffing, patient flow and patient satisfaction? Are you looking for novel ways to improve your metrics and patient satisfaction scores? Contact us today.
SOURCES:
1Ye F, Parast L, Hays RD, Elliott MN, Becker K, Lehrman WG, Stark D, Martino S. Development and validation of a patient experience of care survey for emergency departments. Health Serv Res. 2022 Feb;57(1):102-112. doi: 10.1111/1475-6773.13853. Epub 2021 Aug 12. PMID: 34382685; PMCID: PMC8763294.
2Rowe A, Knox M. The Impact of the Healthcare Environment on Patient Experience in the Emergency Department: A Systematic Review to Understand the Implications for Patient-Centered Design. HERD. 2022 Dec 21:19375867221137097. doi: 10.1177/19375867221137097. Epub ahead of print. PMID: 36541114.
3 Aleksandrovskiy I, Ganti L, Simmons S. The Emergency Department Patient Experience: In Their Own Words. J Patient Exp. 2022 May 20;9:23743735221102455. doi: 10.1177/23743735221102455. PMID: 35619989; PMCID: PMC9128049.
Please correct the following fields before submitting:
- Field Name is required
- Field Email is required